Moisturized Breathing Air
In a typical breathing process, air passes through the nose and mouth, getting filtered and humidified before reaching the lungs. This ensures warm and moisturized air for breathing.
However, laryngectomy patients lack this natural filtration and humidification process due to a surgically placed stoma. Consequently, their lungs produce more mucus to compensate, leading to potential issues like bloody sputum and increased susceptibility to bronchitis.
To counter these problems, it’s crucial for laryngectomy patients to maximize the moisture in their breathing air.
The stoma needs to be sprayed with sterile water or a saline solution 3 to 4 times per day.
Ensuring proper moisture levels in the air is vital for laryngectomy patients, and seeking guidance from healthcare professionals is essential in this regard.
One effective method is to use a cool-mist humidifier in the bedroom to maintain moisture levels during sleep. Regular maintenance, including daily water changes and periodic cleaning with a diluted bleach solution, helps prevent bacterial growth.
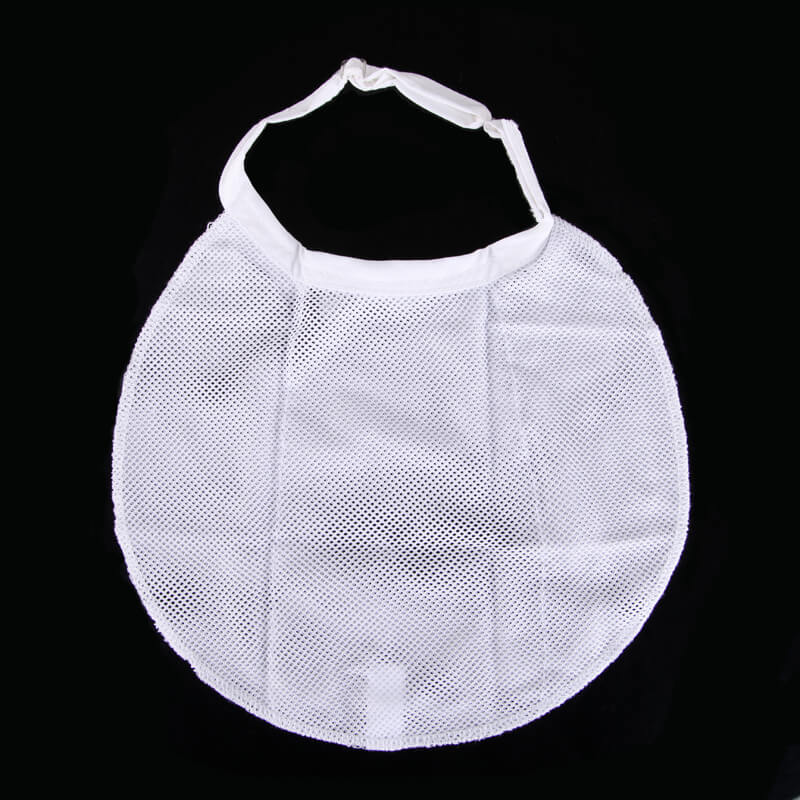
Additionally, patients can enhance moisture retention by wearing stoma bibs, foam protectors, scarves, turtleneck shirts, or sweaters. These accessories help trap moisture in the lungs, reducing moisture loss during exhalation.

The stoma bibs can become portable humidifiers just by dampening them with clean saline water.
Other options include wearing a soft stoma vent, which needs to have the proper size for each patient.
While stoma care is critical, cleaning and caring for your electrolarynx is essential too. Speech aid devices need to be kept in good condition to reassure they are operating correctly and to prevent infection.
It is very common for patients to feel anxious about returning to their daily routines. However, patience is necessary. The whole respiratory system, especially the trachea and lungs will adapt and improve within 3 to 4 months after the laryngectomy.
Check out some of our Stoma Care Products and Labex Electrolarynx Devices!
Please consider joining our Labex Support Center for Laryngectomee FB group:
https://www.facebook.com/groups/801546370394224.



